Learn About Depression


Dr Matthew Whalley

Dr Hardeep Kaur
Published
Everyone feels ‘down’ from time to time, but depression is more than that. When you are depressed your low mood can last for weeks at a time. While mild depression might not stop you from living your life, severe depression can make you feel suicidal and unable to function normally. It is thought that between 3 and 7 people out of every 100 will experience depression every year [1, 2]. The good news is that there are many effective psychological and medical treatments for depression.
What is depression?
If you are depressed, you may have low moods for long periods of time. Common symptoms of depression include:
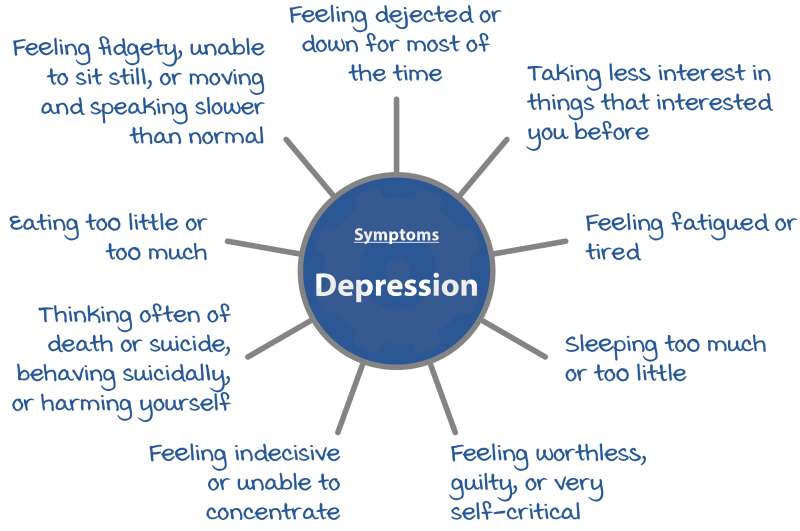
Some people have an episode of depression once and recover, other people have many episodes of depression throughout their life. Further episodes can be more easily triggered if you have had depression before.
What is it like to have depression?
People who suffer from depression often find that their negative thoughts and mood interfere with their work and social life. Tanya’s story shows what it can be like:
Tanya’s depression
I was thirty-four when I first decided to see a therapist. My relationship with Phil had ended after four years, even after I had moved cities to be with him. I had been feeling unhappy before the breakup, but after it happened I was devastated, and things just got worse over the next year. Sometimes I felt so sad that I just couldn’t stop crying, and other times I would feel hollow and empty. When I spoke to friends on the phone they would reassure me that things would pick up, but it didn’t happen.
I used to be quite an active and hopeful person, but now I was struggling to motivate myself. I took a lot of time off sick from work because I couldn’t face it, and when I was there I couldn’t concentrate. I worried that my manager would get rid of me, but I couldn’t summon the motivation to do anything about it. I stayed home whenever I could and didn’t want to see anyone. I couldn’t get enthused about anything, couldn’t be bothered to cook properly, and wasn’t doing anything I enjoyed because nothing seemed worth doing. I would often wake during the night and find myself thinking over all the things that had gone wrong in my life and wondering why they happened. I felt completely hopeless about the future, and was sure that the breakup meant that I would never have children. Sometimes I would hear my mother’s voice in my head saying “You’ll never make a success of your life.”
Do I have depression?
Depression should only be diagnosed by a mental health professional or a doctor. However, answering the screening questions below can give you an idea of whether you might find it helpful have a professional assessment.
| Do you feel bad about yourself, think of yourself as a failure, or feel hopeless? | |||
| Never | Occasionally | Sometimes | Often |
| Do you find it a struggle to stay interested in your hobbies or activities? | |||
| Never | Occasionally | Sometimes | Often |
| Do you feel restless or agitated, or have trouble sleeping? | |||
| Never | Occasionally | Sometimes | Often |
| Do you feel tired, exhausted or lacking in energy? | |||
| Never | Occasionally | Sometimes | Often |
| Do you struggle to motivate yourself to do things? | |||
| Never | Occasionally | Sometimes | Often |
If you answered ‘sometimes’ or ‘often’ to most of these questions, you could be experiencing the symptoms of depression. This is one of the factors that a psychologist will use to make a diagnosis.
What causes depression?
There is no single cause for depression. You are more likely to experience depression if you have had [3]:
Stressful life events which kick-start the depression.
A habit of thinking negatively.
Early experiences which made you vulnerable to depression.
There may be genes which make you more likely to develop emotional problems in general, but there is not yet any strong evidence which indicates that specific genes make you more likely to develop depression [4].
What keeps depression going?
CBT proposes that the reason why some people’s depression doesn’t get better by itself is because they are struggling with a mixture of interpreting things in unhelpful ways and acting in ways that are self-defeating. It has a lot to say about why depression might not get better by itself, but some of the most important reasons are to do with:
Treatments for depression
Psychological treatments for depression
Depression is one of the most extensively-researched emotional problems, and there are many effective psychological treatments. One recent review found that all of the therapies listed below can be effective in the treatment of adult depression [5]:
Interpersonal psychotherapy (IPT)
Life-Review Therapy
Problem-Solving Therapy
Psychodynamic Therapy
In addition, Mindfulness Based Cognitive Therapy (MBCT) has been shown to prevent relapse in people who have recovered from depression, or who have had three or more episodes of depression [6].
Medical treatments for depression
The National Institute for Health and Care Excellence (NICE) recommends SSRI-type antidepressant medication for depression. If a person does not respond to SSRIs, other drug classes including tricyclic antidepressants can be considered, and antidepressant treatment can be augmented with lithium or antipsychotic drugs [7].
References
Stansfeld, S., Clark, C., Bebbington, P., King, M., Jenkins, R., & Hinchliffe, S. (2016). Chapter 2: Common mental disorders. In S. McManus, P. Bebbington, R. Jenkins, & T. Brugha (Eds.), Mental health and wellbeing in England: Adult Psychiatric Morbidity Survey 2014. Leeds: NHS Digital.
Kessler, R. C., Chiu, W. T., Demler, O., & Walters, E. E. (2005). Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey Replication. Archives of General Psychiatry, 62(6), 617-627.
Beck, A. T., Bredemeier, K. (2016). A unified model of depression: integrating clinical, cognitive, biological, and evolutionary perspectives. Clinical Psychological Science, 4(4), 596-619.
Culverhouse, R. C., Saccone, N. L., Horton, A. C., Ma, Y., Anstey, K. J., Banaschewski, T., ... & Bierut, L. J. (2018). Collaborative meta-analysis finds no evidence of a strong interaction between stress and 5-HTTLPR genotype contributing to the development of depression. Molecular psychiatry, 23(1), 133-142.
Cuijpers, P., Quero, S., Noma, H., Ciharova, M., Miguel, C., Karyotaki, E., ... & Furukawa, T. A. (2020). Psychotherapies for depression: a network meta-analysis covering efficacy, acceptability and long-term outcomes of all main treatment types. World Psychiatry.
Spijker, J. A. N., De Graaf, R., Bijl, R. V., Beekman, A. T., Ormel, J., & Nolen, W. A. (2002). Duration of major depressive episodes in the general population: results from The Netherlands Mental Health Survey and Incidence Study (NEMESIS). The British Journal of Psychiatry, 181(3), 208-213.
National Institute For Health And Care Excellence (2009). Depression in adults: recognition and management. Retrieved from: https://www.nice.org.uk/guidance/cg90/resources/depression-in-adults-recognition-and-management-pdf-975742638037
About this article
This article was written by Dr Matthew Whalley and Dr Hardeep Kaur, both clinical psychologists. It was last reviewed on 2021/12/08.
Get sent more useful pieces like this!
Sign up to our monthly newsletter full of helpful ideas, tools, and tips for mental health professionals like you. You'll find out about our latest resources, and you can also read our reviews of the latest research.
It's completely free and you can unsubscribe at any time.

-800.png)

-800.png)